|
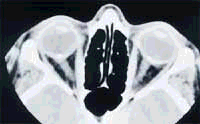
Fig 1
|
||
Radiological
Diagnosis
OPTIC disc drusen
Discussion:
CT Orbits show calcification at the head of the optic nerves bilaterally. No other significant findings were noticed.
Friesen et al described the first case of Optic Disc Drusen. They mentioned that in younger patients, drusen frequently lie deep beneath the surface of the elevated nerve head, where they can not be directly identified by ophthalmoscopy. Therefore, CT is the choice of investigation, because of their calcium content.
Drusen is common and have an incidence of 3.4 to 20 per 1000 of the general population. Most patients are asymptomatic, but some have transient visual obscuration, slowly progressive enlargement of visual field defect or simply dimness of vision.
Pathogenesis of drusen of the optic nerve has long been a subject of dispute. Seitz and Kersting postulated that drusen originated from axoplasmic derivatives of degenerating nerve fibres. Spencer in his Jackson Memorial Lecture proposed that the axoplasmic transport alteration might be the basic pathogenetic mechanism for the formation of drusen in the optic nerve and suggested that this alteration might be related to a genetically determined small crowded optic nerve head.
Mark (88) suggested that abnormal axonal metabolism leads to intracellular mitochondrial calcification. Some axons rupture and mitochondria are extruded into the extracellular space. Calcium is heavily deposited in the extracellular mitochondria. Small calcified microbodies are produced and calcium continues to deposit on the surface of these nidi to form a drusen.
References:
-
Friesen L,Scholdstrom G, Svendsen P: Drusen of the optic nerve head: verification by Computerised tomography. Arch Ophthalmol 1978; 96:1611-1614.
-
Seitz R. Die intraokularen Drusen. Klin Monatsbl Augenheilkd 1968;152 :203-11
-
Spencer WH. Drusen of the optic disc and aberrant axoplasmic transport. Ophthalmology 1978; 85:21-38.
-
Tso MOM. Pathology and Pathogenesis of Drusen of the Optic Nervehead. Ophthalmology 1981; 88:1066-1080